Dental implants are a highly dependable way to replace missing teeth, but their long-term success relies on healthy gums and bone. How gum disease impacts dental implants is a critical topic because gum disease can disrupt healing, weaken support around implants, and raise the risk of complications. Knowing how gum disease develops, how gum disease impacts dental implants over time, and the steps you can take to prevent problems helps you protect your investment and your smile.
What Is Gum Disease?
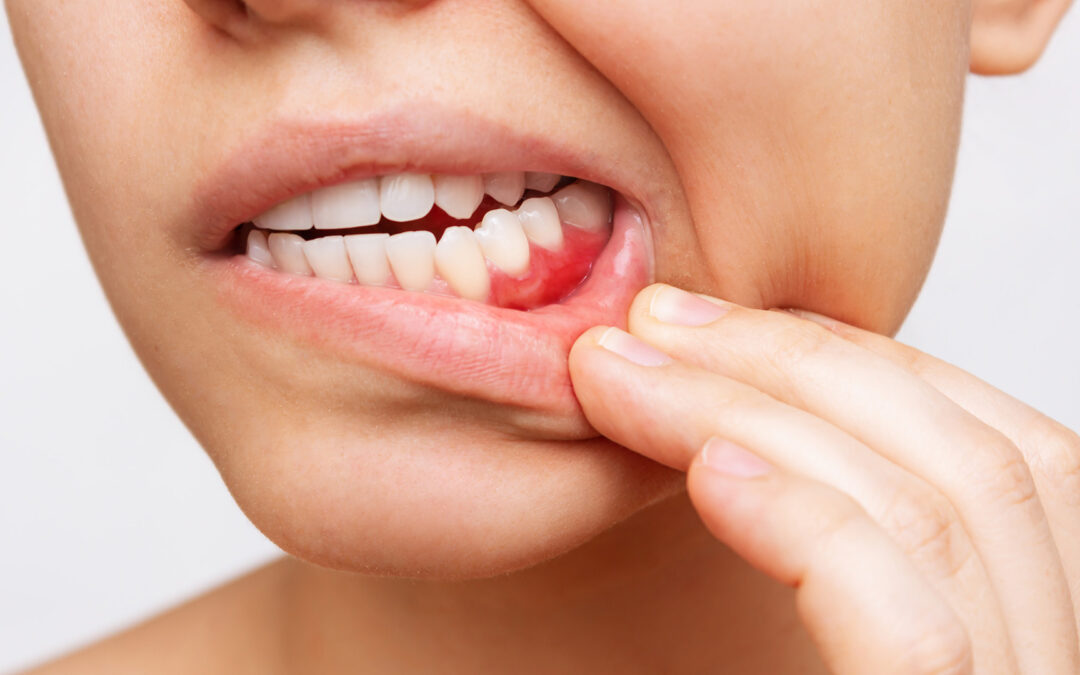
Gum disease is an infection and inflammation of the tissues that support teeth. It starts as gingivitis, a reversible condition caused by plaque buildup along the gumline. Without treatment, it can progress to periodontitis, a more serious stage that damages the bone and connective tissue anchoring the teeth. In periodontitis, deep pockets form between the teeth and gums, creating areas where bacteria thrive and continue to destroy the supporting structures.
Common warning signs include red, swollen, or tender gums; bleeding when brushing or flossing; persistent bad breath; gum recession; tooth sensitivity; and loose or shifting teeth. Early gum disease is often painless, which is why regular dental checkups are essential for early detection and intervention.
Risk factors include poor oral hygiene, smoking or vaping, diabetes, a family history of periodontal disease, hormonal changes, medications that reduce saliva flow, clenching or grinding, and chronic stress. Diets high in sugar and irregular dental visits can also increase your risk.
How Gum Disease Affects Dental Implants
Healthy gums and adequate bone are vital for implant success. Active gum disease can reduce the predictability of the healing process known as osseointegration, the fusion of an implant with the jawbone. Inflammation elevates bacterial levels and interferes with tissue regeneration, making early healing less reliable.
Gum disease around implants typically appears as mucositis, which is inflammation limited to the soft tissue. If not addressed, it can progress to peri-implantitis, a condition that involves inflammation and bone loss. Peri-implantitis resembles advanced periodontitis and can lead to progressive bone destruction around the implant threads, implant mobility, and ultimately implant failure.
When inflammation breaks down the seal between the gum tissue and the implant, bacteria can penetrate deeper areas, triggering an immune response that accelerates bone resorption. Factors such as smoking, uncontrolled plaque, and systemic conditions like poorly managed diabetes amplify this response and make peri-implant tissues more susceptible to breakdown. Understanding gum disease and dental implants together is essential, because the same bacteria that cause periodontal disease can compromise implant health if not controlled.
Evaluating Candidacy for Dental Implants with Gum Disease
A thorough periodontal and oral health evaluation is the first step in determining whether implants are appropriate. Your dentist or periodontist will review your medical history, measure pocket depths, check for bleeding and tooth mobility, and evaluate bone levels using imaging such as digital X-rays or 3D cone beam scans. Stable gum health, sufficient bone volume, and consistent home care habits are critical for candidacy.
Active gum infection must be treated before implant surgery. Reducing bacterial load and controlling inflammation improves healing and long-term stability. Treatment often includes professional cleanings, scaling and root planing, and targeted antimicrobial therapies. In some cases, bone grafting or soft tissue procedures may be recommended before or during implant placement to rebuild lost support.
Your provider will stage the disease, identify contributing risk factors such as diabetes or tobacco use, and develop a personalized timeline. A staged plan, disease control, re-evaluation, then implant placement, often provides the best chance for long-term success. This approach addresses gum disease and dental implants as a combined consideration, ensuring the mouth is healthy enough to support predictable implant outcomes.
Treatment Options for Gum Disease
Non-surgical therapy is the first line for most patients. Scaling and root planing removes plaque and tartar above and below the gumline and smooths root surfaces to discourage bacterial reattachment. Adjunctive therapies may include localized antibiotics, antimicrobial mouth rinses, and laser-assisted treatments to reduce bacteria and inflammation. Consistent home care and regular professional maintenance are essential after initial therapy.
For advanced disease, surgical care may be needed. Options include flap surgery to access and clean deep pockets, osseous surgery to reshape irregular bone, guided tissue regeneration and bone grafting to rebuild lost support, and soft tissue grafts to treat recession and improve tissue quality around teeth or implants. When peri-implantitis is present, specialized procedures and implant surface decontamination are used to control infection and, when feasible, regenerate lost bone.
After treatment, the focus shifts to maintaining gum health to protect both natural teeth and implants. This involves meticulous brushing and interdental cleaning, using antimicrobial rinses as directed, scheduling regular periodontal maintenance visits, and monitoring systemic factors such as blood sugar control. Staying on your maintenance schedule significantly lowers the risk of recurrence.
Preventing Gum Disease for Better Implant Outcomes
Daily habits are the foundation of prevention. Brush twice a day with a soft-bristled toothbrush and fluoride toothpaste, and clean between teeth once a day with floss, interdental brushes, or a water flosser. Around implants, many patients benefit from implant-safe interdental brushes and super floss to thoroughly clean without damaging the restoration.
Routine checkups and professional cleanings help catch early signs of gum disease and peri-implant problems. After implant placement, your dentist may recommend more frequent periodontal maintenance, especially if you have a history of gum disease. Regular evaluations allow your dental team to adjust your home care and treat inflammation early.
Lifestyle choices strongly influence gum and implant health. If you smoke or vape, seek support to quit; tobacco use significantly increases the risk of peri-implantitis and implant failure. Maintain a balanced diet rich in protein, vitamins C and D, and minerals that support healing and bone metabolism. Manage systemic conditions such as diabetes, reduce stress, get adequate sleep, and wear a nightguard if you clench or grind. These steps help control inflammation and protect implants over the long term. For anyone researching how gum disease impacts dental implants, prevention is the most reliable way to safeguard the tissue and bone that keep implants stable.
Key Differences: Healthy Implants vs. Implants Affected by Gum Disease
| Feature | Healthy Implant | Implant with Mucositis/Peri-implantitis |
| Gum appearance | Pink, firm, no bleeding | Red, swollen, bleeding on brushing or probing |
| Pocket depth | Shallow, stable | Deepening pockets around the implant |
| Bone levels | Stable on X-rays | Progressive bone loss visible on imaging |
| Symptoms | Comfortable, functional | Tenderness, bad taste or breath, possible mobility |
| Prognosis | Excellent with routine care | Guarded without timely treatment |
When to See a Dentist
- Bleeding gums or persistent bad breath
- Sensitivity or tenderness around an implant
- Gum recession or a change in how an implant crown feels when biting
- Redness, swelling, or drainage near an implant
- Missed maintenance visits or difficulty keeping implants clean at home
Early evaluation allows for conservative treatment and better outcomes. Waiting can lead to deeper infection and more complex care.
The Bottom Line
Gum disease can jeopardize dental implants by disrupting healing, breaking down the tissue seal, and accelerating bone loss. The good news is that careful planning, effective treatment of gum disease before surgery, and consistent maintenance greatly improve implant success. Partner with your dental team for a personalized plan that includes risk assessment, tailored home care, and regular periodontal maintenance. With healthy gums and vigilant follow-up, your implants can stay strong and comfortable for years to come. Keeping the focus on gum disease and dental implants as interconnected issues helps you make informed decisions and prioritize the habits that support long-term stability.