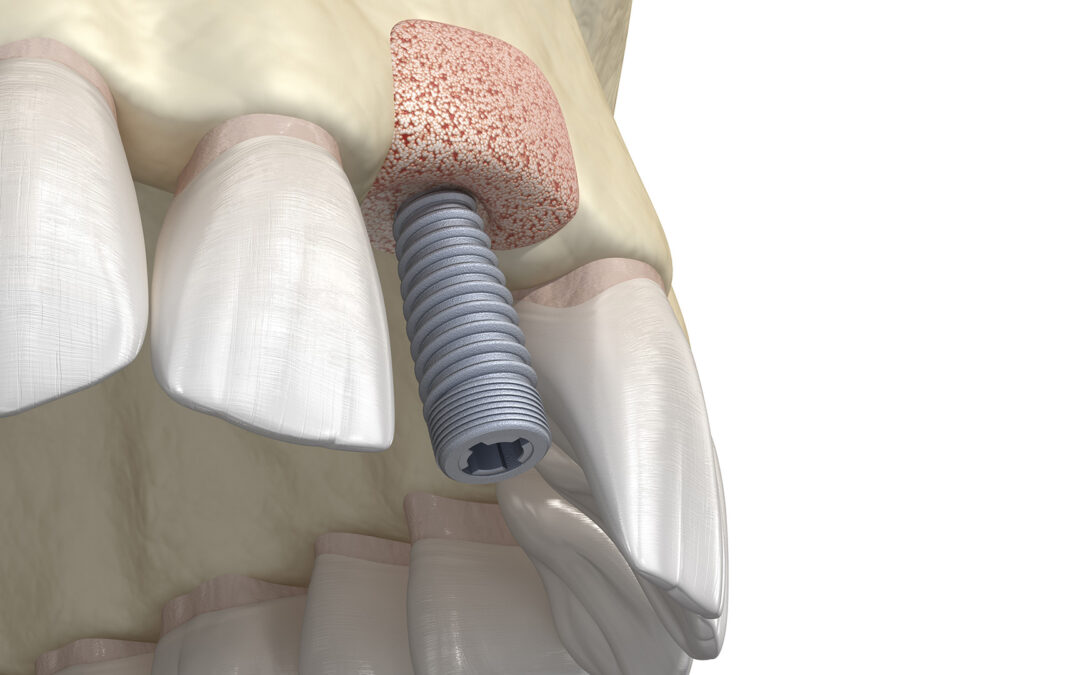
Jaw bone grafting restores lost or weakened bone so it can support healthy teeth, dental implants, and overall facial structure. In an oral bone graft, clinicians collaborate with trusted oral surgeons and restorative dentists to plan grafts that complement orthodontic or implant treatment. Below, we outline what jaw bone grafting is, why it may be recommended, how the procedure works, and what to expect during recovery, so you can make informed decisions about your oral health. When performed thoughtfully, a bone graft mouth procedure can help rebuild areas affected by tooth loss or gum disease and improve long-term oral function.

What Is Jaw Bone Grafting?
Jaw bone grafting adds or regenerates bone where volume or density has diminished. The aim is to build a stable foundation for teeth and dental implants, while supporting natural facial contours. An oral bone graft is tailored to the unique demands of the mouth and may be used to improve implant sites or stabilize teeth weakened by bone loss.
Common graft materials include:
- Autograft: your own bone, often from the chin or another donor site
- Allograft: processed donor bone
- Xenograft: bone from animal sources, typically bovine
- Alloplast: biocompatible synthetic materials that encourage bone growth
Your provider will recommend the option best suited to your health, anatomy, and treatment plan. In a bone graft mouth procedure, material choice and placement technique are selected to promote predictable healing and integration with your natural bone.
Grafting in the jaw is tailored to the unique demands of the mouth, chewing forces, precise implant positioning, and proximity to the sinuses. Techniques such as ridge augmentation, socket preservation, and sinus lifts are customized to your jaw anatomy and the timing of orthodontic or implant therapy. These approaches are part of comprehensive care planning for jaw bone grafting, ensuring that oral bone graft outcomes align with long-term restorative or alignment goals.
Why Is Jaw Bone Grafting Necessary?
Several conditions can reduce jaw bone volume, including periodontal disease, long-standing tooth loss, trauma, congenital defects, and infection. Jaw bone grafting is often recommended to stabilize an area before orthodontic alignment or implant placement. By reinforcing compromised sites, an oral bone graft can improve tooth stability and prepare for future restorations.
Dental implants require strong, healthy bone to integrate and remain secure. When bone is insufficient, an implant may not be feasible or could fail prematurely. By rebuilding deficient areas, a bone graft mouth procedure helps create predictable implant outcomes and long-term stability for crowns, bridges, or overdentures.
After a tooth is removed, the surrounding bone naturally resorbs over time. This can alter your bite, impact facial aesthetics, and complicate future restorations. Jaw bone grafting can preserve the ridge immediately after extraction (socket preservation) or reconstruct areas that have thinned, supporting both function and appearance. In cases of advanced sinus pneumatization, sinus lift techniques can increase vertical bone height for implant placement.
The Jaw Bone Grafting Procedure
While specifics vary by case, the typical process includes:
- Assessment and imaging (X-rays or 3D scans) to determine graft size and placement
- Site preparation, including careful cleaning and shaping
- Placement of the graft material and, when indicated, a protective membrane
- Stabilisation with sutures and detailed post-operative instructions
For sinus lift procedures, the sinus floor is gently elevated and graft material is placed to increase vertical bone height, creating space and support for future implants. This is a specialized form of oral bone graft aimed at reinforcing the upper jaw.
Your comfort is a priority. Local anesthesia is typically used, and some patients may opt for sedation depending on the complexity of the procedure and personal preference. Your clinician will review your medical history, discuss options, and recommend a safe, personalized plan.
Post-procedure care focuses on protecting the graft as it begins to heal. Typical guidance includes:
- Take prescribed medications exactly as directed
- Use cold compresses during the first 24-48 hours to reduce swelling
- Choose soft foods and avoid chewing on the grafted side
- Keep the area clean with gentle rinsing as instructed; avoid vigorous spitting
- Do not smoke, vape, or use straws during early healing
- Attend all follow-up visits with your surgical and dental providers
Following these steps helps ensure a bone graft mouth site remains undisturbed, promoting healthy integration.
Recovery and Expected Outcomes
Initial recovery typically takes 1-2 weeks, though full graft maturation generally occurs over 3–6 months. During this time, the graft integrates with your natural bone, strengthening the jaw for future orthodontic movement or implant placement. With appropriate care, jaw bone grafting can offer durable support for replacements and improve chewing function.
Healthy healing usually involves decreasing swelling within a few days, manageable discomfort, pink and healthy gum tissue, and no persistent drainage. Contact your care team promptly if you experience any of the following:
- Prolonged or increasing pain
- Fever or unusual swelling
- Persistent bleeding
- Graft exposure or membrane loosening
- Persistent numbness
Long-term success depends on consistent follow-up and excellent oral hygiene. Regular check-ups, professional cleanings, and daily home care, twice-daily brushing, interdental cleaning, and a balanced diet, help maintain healthy bone and gums. When coordinated with comprehensive treatment planning, oral bone graft procedures create a reliable foundation for precise tooth movement and durable implant restorations. Understanding the indications, process, and recovery for jaw bone grafting empowers you to make informed choices that support a functional, confident smile.